“As long as the baby is healthy, that’s all that matters.”
Many well-meaning people say this in response to moms sharing their traumatic childbirth experiences. Please don’t be this person. It devalues the mom’s experiences, and echoes the many ways that we become reduced to our role as moms, and are encouraged to be selfless in honor of our children.
I know because it happened to me. I hadn’t given much thought to how I would deliver my first child until I went to my child birthing class. My mom had done Lamaze with me, so I searched for a Lamaze class, too. I had no idea there were so many different child birthing methods. As I learned more, I became intrigued, and decided that hey, maybe I did actually care about how I’d birth my baby. It was during this class that I also learned about doulas, and decided to search for one. We came up with my birth plan together—a document that was almost five pages long.
I made a playlist to listen to while in the hospital, and eagerly packed my bags for the hospital. Soon after, things would spiral. At 37 weeks, my doctor decided to induce me because my son was measuring small. When I asked her why, or if we could wait just a little longer, she shrugged it off and said this would be better for us. Plus, she noted, I’m going on vacation around your due date, and I want to be sure I’ll be here to deliver the baby. If I could have tapped myself here, I would have screamed to ask what my options were. But of course, I had no idea what was about to happen. When I discussed it with my Lamaze teacher, she smiled weakly at me and told me what to look out for. I halfway listened—there was no way I was having a C-section, so I didn’t need to prepare.
The induction process with my son was one of the most traumatic experiences I’ve ever had. The contractions, spurred on by increasingly high levels of Pitocin, were beyond painful. But I was determined to have my baby naturally—the nurse even wrote it on the dry erase board in my room. As the level of Pitocin continued to climb and the pain intensified, the nurses kept asking if I wanted pain relief. I shook my head and concentrated on envisioning my happy place as I breathed through the contractions that would eventually come every 30-60 seconds. My hopes of a natural birth continued to slip away as I made no progress in labor. As the day wore on, everything that my Lamaze teacher told me began playing in my head. As the Pitocin levels increased and my contractions grew stronger, the nurses became worried about the baby’s heart rate. After 14+ hours of labor, I knew the C-section was inevitable so I decided to get the epidural so I could at least be comfortable before the surgery. My husband tried to keep an upbeat attitude but I knew he was getting worried.
My fears were confirmed. Without attempting any movement or any natural interventions, the nurses and doctors insisted that an emergency C-section was necessary. Again, if I could have tapped myself, I would have pumped the breaks and asked to move around, to squat, for natural interventions. I would have also insisted that my doula not leave until I delivered the baby so she could have helped with these interventions. But alas, none of those things happened. After 17 hours of labor, 1.5 centimeters of dilation and fearing for my life while on the operating table, I delivered my son through emergency C-section. My husband said he’d never seen me look so terrified.
The trauma of that experience led me to question if I wanted to have another child. It took me four years to get to the point of wanting to try for another baby. Once I became pregnant, I was determined to try for a vaginal birth after C-section, or VBAC. Many doctors decline to try VBACs because of the risk of uterine rupture, so I knew it would be a challenge to find a doctor that supported my decision. To my surprise, I found a doctor that supported my journey to VBAC. I asked her at multiple appointments and her answer remained the same. She wholeheartedly encouraged it and was excited to try it.
That all changed when my daughter began measuring small at my appointments. I was sent to a maternal fetal specialist, who began questioning if my VBAC journey would actually happen. They said it was an option, but only if my doctor agreed. To my surprise, she did what is called a “bait and switch.” We had a horrible conversation where it was clear she was trying to scare me and present the absolute worst case scenario of what could happen with a VBAC. Uterine ruptures do happen, but the risk is extremely low. There are also varying levels of uterine ruptures, which can also happen with C-sections. I know all of this because I did my research before asking her these questions. When I asked her about the potential risks of a repeat C-section, she grew quiet. It was at that moment that I decided to end my relationship with her and seek a new doctor. I promised myself that after my previous birthing experience, I would always speak up for myself and be my own advocate.
At this point, I was 29 weeks pregnant. Most doctors are not necessarily jumping to accept patients this far along into their pregnancies, especially patients wanting to have a VBAC. It was very difficult to find a doctor, particularly because my MFM became less hopeful that a VBAC was possible. I was devastated. But this time around, it was more than just about clinging to birthing my daughter one specific way.
I wanted to feel empowered. I wanted to be present. I wanted to feel connected to my body. That had nothing to do with whether I delivered her vaginally or had a repeat C-section. So I began leaning into the idea that a C-section might happen. This was a stark difference from my first pregnancy, when I refused to consider that a C-section could happen. Learning more about C-sections and exploring my options made me feel empowered. I began to research gentle C-sections, and was pleasantly surprised when my new doctor was completely onboard with this option.
I made a gentle C-section birth plan—again, something I’d never considered when writing my first birth plan. There are many different options for gentle C-sections—the most important thing is talking to your doctor and making sure that they are aware of what you want. It was important to me to see my daughter being born. I’d felt so disconnected from my son’s birth, and I knew this was an important part of my healing. My new doctor and I talked about what I would need to heal. One of the most traumatizing aspects of my first C-section was feeling so out of control—I had no idea what was happening during the surgery. To make things worse, the doctors and nurses were talking about their weekend plans and having normal conversations as I tried my best to not show how terrified I was.
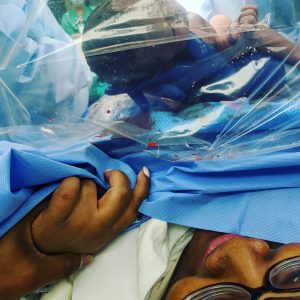
So my doctor agreed to introduce herself and have everyone else in the room do the same. During the surgery, she assured me that she would give me a verbal rundown of every single thing that she did. A clear drape was dropped as my daughter was being born, which allowed me to see her. It is a moment I will never forget. I was able to see my daughter take her first breath. I was able to make a playlist which was played in the operating room, and my daughter was born to the song “Yellow” by India.Arie, my favorite singer. My doctor gave me the option to hold her but I didn’t have the energy after the delivery. I also had the option to breastfeed in the operating room—the nurses made sure that my hospital gown was positioned in order for this to happen. But I was so exhausted and overwhelmed, so I waited until I got back to the recovery room. My daughter latched immediately—an experience I didn’t have after my first birth. The trauma from the surgery was too much for me to handle, and my son spent his first night in the nursery.
Although I didn’t end up with a VBAC, I am so grateful for my gentle C-section. It was the experience I didn’t know I needed. My doctor worked with me right up until the morning of the surgery, allowing me to make the final decision to not get induced for a second time. We agreed that a long labor would not be good for me or my daughter. I thought that I would feel defeated when I made that choice, but all I felt was empowerment. I had a doctor that presented me with multiple options, encouraged me to do my own research and answered every single question that I had.
Ultimately, my birthing experience was the healing that I needed. It does matter how we birth our children. We deserve to birth in the way that makes us feel the most empowered. During my first birth, I felt like all of the decisions were being made for me. My gentle C-section allowed me to have an active role in a procedure that happened to my body. Giving birth is about more than just birthing a baby. We are also birthed as parents. This second time around, my parenting journey began with advocacy, hope, and restoration.